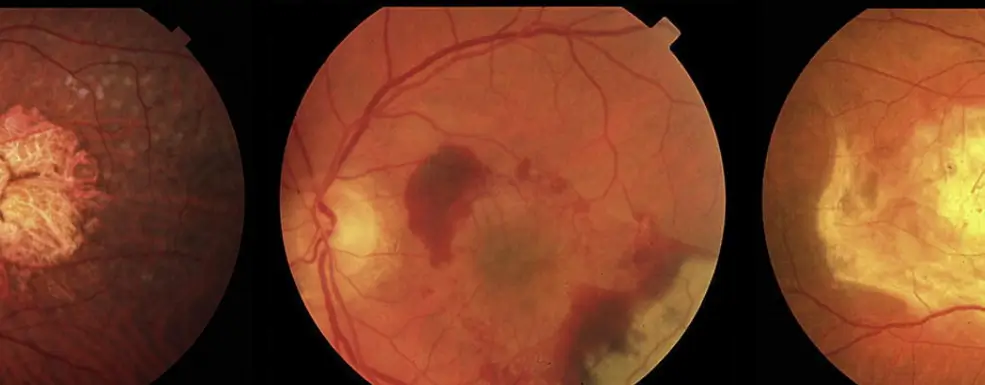
Overview
Age-related macular degeneration (AMD) is a common eye condition and one of the leading causes of vision problems among older adults. It affects the macula, a small but critical part of the retina responsible for sharp, detailed central vision. Damage to this area can interfere with essential visual tasks such as reading, recognizing faces, driving, and seeing fine details.
According to global health data, AMD is among the leading causes of blindness in developed countries and ranks as the third most common cause of blindness worldwide after cataract and glaucoma.
What Happens in Age-Related Macular Degeneration
The macula allows people to see fine details in the center of their visual field. When AMD develops, damage to this area gradually reduces central vision while peripheral vision usually remains intact. As a result, people may appear to see normally but struggle with tasks requiring detailed vision, such as reading small text or identifying faces.
Many individuals with AMD develop small yellow-white deposits in the macula called drusen, which are often associated with early stages of the disease. However, not everyone with AMD develops these deposits.
Types of Age-Related Macular Degeneration
AMD occurs in two primary forms: dry AMD and wet AMD.
Dry AMD
The most common form. Cells of the macula gradually break down over time, causing blurred central vision and eventual blank spots in the visual field. Symptoms may be subtle in early stages. A small proportion develop geographic atrophy, a severe form causing significant vision loss.
Wet AMD
Less common but more aggressive. Abnormal blood vessels grow beneath the retina and can leak blood or fluid into the macula, causing scarring and rapid vision damage. Vision loss can develop over days or weeks, making it a more urgent condition.
Risk Factors
Age is the most significant risk factor for developing AMD. As people get older, the likelihood of the disease increases. Other factors may also raise the risk:
- Cigarette smoking
- Cardiovascular risk factors such as high cholesterol
- Family history of AMD
- Diet low in green leafy vegetables, fruits, fish, and nuts
Symptoms
Symptoms vary depending on the stage and type of AMD. Unlike many other eye conditions, AMD usually does not affect peripheral vision — individuals may retain side vision even in advanced stages.
Wet AMD symptoms often appear more suddenly and may include straight lines appearing crooked or distorted, blurred or distorted images, and the development of a central blind spot.
Some people with advanced AMD may also experience visual hallucinations, seeing patterns or shapes that are not actually present.
Diagnosis
Diagnosis typically involves a comprehensive eye examination performed by an ophthalmologist. The evaluation may include:
- Medical history review
- Visual acuity testing
- Dilated eye examination to observe the retina and macula
- Imaging tests to confirm retinal changes or detect abnormal blood vessels
Treatment Options
Treatment depends on the type and stage of AMD.
For dry AMD, although there is currently no cure, certain vitamin combinations may slow the progression of the disease. The AREDS formula, developed by the National Eye Institute, includes Vitamin C, Vitamin E, Zinc, Copper, and Beta-carotene or alternatives such as lutein and zeaxanthin. These supplements may reduce the risk of progression to advanced AMD in certain patients.
For wet AMD, the primary treatment is anti-VEGF therapy — injections into the eye that block the growth of abnormal blood vessels and reduce fluid leakage, helping slow or sometimes improve vision loss. Other options may include laser surgery to seal leaking blood vessels or photodynamic therapy using light-activated drugs such as verteporfin, though these are used less frequently today.
Living With AMD
AMD is generally a lifelong condition. While many individuals with early disease never progress to severe vision loss, those with advanced AMD may require visual aids to maintain independence. Low-vision aids may include:
- Magnifying glasses or spectacles
- Handheld magnifiers
- Computer screens with large text
- Books and devices designed for low vision
Research and Future Directions
Research centers dedicated to AMD are investigating its complex causes and exploring new approaches to prevention and treatment. Key areas of study include:
Cell Biology
Study of retinal and retinal pigment epithelial cell biology to better understand how and why macular cells degenerate over time.
Inflammation & Metabolism
Investigating how inflammatory and metabolic processes contribute to AMD onset and progression.
Genetics
Identifying genetic factors that increase susceptibility to AMD, enabling earlier detection and personalized treatment strategies.
New Therapies
Development of neuroprotection strategies and novel medications aimed at slowing progression and improving patient outcomes.
Scientific References
Harvard Medical School. Macular Degeneration – A to Z. Harvard Health Publishing.
Available at: https://www.health.harvard.edu/diseases-and-conditions/macular-degeneration-a-to-z
Harvard Medical School – Department of Ophthalmology. Age-Related Macular Degeneration (AMD) – Center of Excellence.
Available at: https://eye.hms.harvard.edu/amd
